Summary
Uveitis, inflammation of the eye’s middle layer, can spread quickly and may lead to blindness if untreated. This condition varies in intensity and may impact one or both eyes. Uveitis can develop from multiple causes like trauma, infections, cancer, or autoimmune diseases, with some triggers originating within or outside the eye. Recognizing the symptoms – such as redness, tearing, and iris color changes – is crucial. Proper diagnosis may entail a comprehensive patient history, physical examinations, and various tests. Treatment demands a proactive and adaptive approach, emphasizing inflammation reduction and pain elimination. Left unchecked, uveitis can severely impair vision, but early treatment offers a promising prognosis.
In the soft glow of my clinic, I looked at Mrs. Thompson, her aged Labrador, Max, nervously pawing his inflamed eye. “Max has uveitis,” I said. “It’s inflammation inside his eye.”
Mrs. Thompson’s face clouded. “Will he lose his sight?” she asked, her voice thinning with worry.
“Not if we act quickly, it’s an aggressive opponent,” I replied. “Our eyes are fragile ecosystems. In Max’s case, the battleground is the uvea. That’s one of the inner layers of his eye; it’s getting inflamed.”
“Why?” she asked, her eyes flitting between me and Max.
“Well, it could be many things,” I said, offering a comforting smile. “Sometimes, it’s trauma or infection. Other times, an unseen foe, cancer or an autoimmune disorder. The task now is to find out and treat accordingly.”
She nodded, her hands clenched onto Max’s leash.
I continued, “Max will need medications to quell the inflammation and pain. We may need to run some tests. This is a fight, but not one we’ll let him face alone.”
She looked at me, trust and hope mingling in her eyes. “What are his chances, doc?”
“Depends on the cause,” I responded, looking at Max’s reddened eye. “If we act promptly, we can manage the inflammation and preserve his vision. The enemy may return, but we’ll be ready.”
Her shoulders drooped in relief, Max’s whine lowering in pitch.
“As always, vigilance is our best weapon,” I concluded. “Uveitis, like many foes, doesn’t announce itself. It creeps in. If Max starts squinting, tearing up, or acting unlike himself, bring him in right away.”
I shook her hand, we now had a plan, a hope. For Max, and every other pet that walked through my clinic doors, we’d wage war against uveitis, one eye at a time.
Introduction
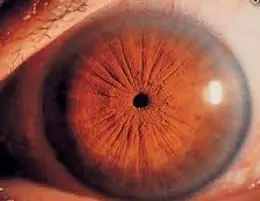
Uveitis is a broad term that refers to inflammation of the middle layer of the eye, also known as the uvea [FIG 1]. This part of the eye includes the iris, ciliary body, and choroid, which carry blood supply, create eye fluid, and hold the structures that help the lens focus on objects.
Uveitis can affect one or both eyes, and the severity of inflammation can vary between eyes. Because the eye is so small, inflammation can quickly spread and lead to blindness if not treated promptly.

What are the Different Types of Uveitis?
The type of uveitis is determined by the location of inflammation within the eye. Anterior uveitis, the most common type, affects the front part of the eye. Signs of anterior uveitis can appear suddenly, and if mild, can sometimes clear up on their own.
Posterior uveitis, though less frequent, can be more severe as it affects the retina, optic nerve [FIG 1], and choroid, causing recurring changes that can last for months or even years. Lastly, panuveitis, which affects all parts of the eye, is rare.
Advertisement
Recognizing the Signs of Uveitis
Uveitis can cause several changes to the eye that include redness, squinting, tearing, and changes in iris color. Some patients might feel pain or discomfort in the affected eye. These changes might not be present in all patients; instead, a constellation of these signs that together support the diagnosis of uveitis.
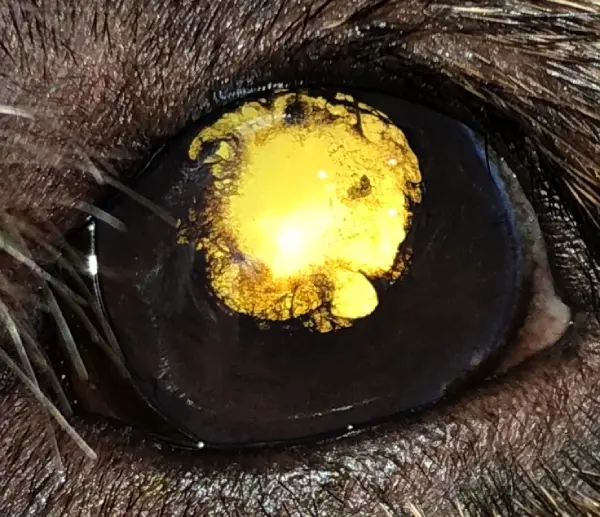
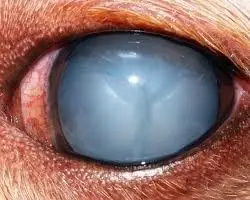
Early signs of uveitis can include conjunctival redness (hyperemia) [FIG 2], frequent eye rubbing, squinting (blepharospasm) [FIG 3], excessive tearing (epiphora) [FIG 4], and light sensitivity (photophobia).
More advanced or chronic symptoms may involve cloudiness of the fluid in the eye (aqueous flare) [FIG 5], corneal deposits (keratic precipitates) [FIG 6], third eyelid elevation, a small pupil (miosis) [FIG 7], pigment deposition on to the lens capsule [FIG 8], scarring within the eye, iris reddening (rubriosis iridis) [FIG 9], darkening of the iris, or bleeding (hyphema) [FIG 11] or pus in the eye (hypopyon) [FIG 10].
In severe untreated cases, these symptoms may progress to cataract [FIG 12] formation, retinal degeneration or retinal detachment [FIG 13], lens displacement (lens luxation or lens subluxation) [FIG 14], globe enlargement secondary to glaucoma (buphthalmia) [FIG 15], globe shrinkage (phthisis bulbi) [FIG 16] or blindness.
Ocular changes that occur secondary to uveitis may develop quickly or slowly over time. These changes can result in an eye that appears different from normal but without affecting vision, or in an eye that appears outwardly normal but without vision, or somewhere in between.
The extent of these changes is usually associated with the severity and duration of the initiating inflammation, further emphasizing the need for early treatment.
Early examination by a veterinary ophthalmologist will identify the parts of the eye affected, initiate treatment that can be expected to reduce or even resolve the changes, perform diagnostic testing to identify the underlying cause, and help to predict the outcome of the changes noted.

What are the Causes of Uveitis?
The causes for uveitis are numerous and can be tricky to identify, but they can be broken down into four major groups that include trauma, infection, cancer (neoplasia), and autoimmune disease (immune-mediated disease).
These groups can be further broken down by those originating from within the eye (ocular causes) or outside the eye (non-ocular causes). This distinction can sometimes be blurred when an underlying disease is known to be present in both locations (e.g. immune-mediated disease, some cancers, infection).
Ocular causes may result from an insult to the cornea or inflammation originating from inside the eye. For example, uveitis can be reflexively triggered following corneal pain due to corneal ulceration, corneal inflammation (keratitis), or rarely, scleral inflammation.
Externally derived causes of uveitis can be the result of corneal pain (eg. penetrating injuries from sharp objects like cat claws) or blunt trauma (eg like a tennis ball hitting the eye).
Infectious processes that cause inflammation are most commonly bacterial, parasitic, or fungal and can reach the eye via the blood supply to the eye, the uvea, or directly into the eye through a corneal injury.
Internally derived sources of inflammation can be the result of tumors or immune-mediated conditions. A common example of immune-mediated disease that causes uveitis that originates from within the eye is lens-induced uveitis.
The lens [FIG 1] is composed of clear protein fibers encased within the clear capsule of the lens. Through injury or advanced cataract [FIG 12] formation, these lens proteins can escape the capsule either microscopically or in large volume.
Interestingly, the lens proteins were encased within the capsule during fetal development before the immune system had fully developed within the eye.
Consequently, lens proteins that escape through the capsule are not recognized by the eye and are attacked as foreign material. As in all parts of the body, foreign material is dealt with through inflammation to either remove it or hide it from the surrounding tissues (in this case the eye).
This is a normal response in the body but when uncontrolled, can have severe consequences within the closed space of the eye.
Other examples of immune-mediated uveitis include Golden Retriever Pigmentary Uveitis (GRPU), and steroid-responsive retinal detachment. Neoplastic diseases that originate from within the eye (primary intraocular tumors) include uveal melanoma, iridociliary adenoma/adenocarcinoma, and feline post-traumatic ocular sarcoma.
Non-ocular causes of uveitis are those conditions or diseases that form away from the eye but can still trigger inflammation within it. These conditions include cancer (neoplasia) that has spread to the eye (eg lymphosarcoma, malignant sarcomas, carcinomas, transmissible venereal tumors, and histiocytic proliferative disorders), immune-mediated diseases of the body (uveodermatologic syndrome, immune-mediated thrombocytopenia, and immune-mediated vasculitis), infection (bacterial, parasitic, or fungal), and idiopathic uveitis, which is a diagnosis made when a specific cause of the uveitis remains unidentified despite thorough examination and testing.
Idiopathic uveitis is the most common diagnosis of uveitis and accounts for 40-60% of cases.
Advertisement
How is Uveitis Diagnosed?
Diagnosing uveitis requires a detailed patient history and a thorough physical examination. The patient’s history can provide invaluable insights into their current and historical health status, the progression of current eye changes, and the response to any treatments that have been previously tried.
In addition, history provided by pet owners will also identify potential risk factors for the patient such as age, breed, environmental conditions, activity level, behaviour, and travel history.
Clinical signs of uveitis are broad and can overlap with many other unrelated ocular diseases. Therefore, by recognizing a pattern in the clinical signs, ruling out eye diseases with similar signs (such as conjunctivitis, dry eye (keratoconjunctivitis sicca), glaucoma, lens displacement (lens luxation), corneal endothelial dystrophy or corneal degeneration, Horner’s syndrome, and high blood pressure (systemic hypertension), and obtaining historical information, clues to the underlying cause are often obtained.
As a frustrating consequence to the small size of the eye, unrelated eye conditions can over time not only cause uveitis, but also develop because of uncontrolled uveitis. Again, this highlights the need for urgent diagnosis and treatment.
If the cause of uveitis is not immediately apparent, further tests may be needed. These can include blood work, infectious disease testing, urinalysis, cytology, biopsy, x-ray (radiography), ultrasound, or advanced imaging like MRI or CT scans. These investigations can help identify systemic diseases or infections that might have triggered the eye inflammation.
Sometimes the specific cause of uveitis cannot be identified despite exhaustive testing.
How is Uveitis Treated?
The treatment of uveitis requires a targeted, aggressive, and often prolonged approach with the flexibility to adjust based on the patient’s response to therapy. The primary goal of treatment is to reduce inflammation and eliminate pain.
The initial treatment might include topical or systemic anti-inflammatory medications, antibiotics, or antifungal drugs, depending on the underlying cause.
Supportive care, such as pain management, frequent check-ups, and careful monitoring of the pet’s overall health, is also crucial. In some instances, surgical intervention may be necessary to manage complications or prevent further damage to the eye. If uveitis is secondary to an underlying systemic disease, addressing that disease is vital for successful treatment of the uveitis.
Advertisement
Conclusion
Uveitis is a severe condition that can lead to vision loss or even blindness if left untreated. With early treatment and targeted therapy, many cases of uveitis can be managed effectively, preventing long-term complications.
The speed of recovery and the likelihood of recurrence depend heavily on the cause and the duration of the inflammation before treatment began. A pet’s age, general health, and other concurrent diseases also play a role in the prognosis.
With proper veterinary care, patient compliance, and regular follow-ups, many pets with uveitis can maintain a good quality of life.

 Pet News
Pet News