Summary
Periodontal disease is one of the most common issues affecting pet dogs, with up to 90% of dogs over the age of 2 years old being affected. Chronic periodontal disease in dogs can lead to dental problems and tooth loss, as well as serious general health problems. Therefore it is important to prevent it through regular daily oral hygiene, routine veterinary check-ups, and professional cleaning as necessary. This article explains the details of periodontal disease, how it occurs, and how it can be prevented and treated.
When Susan brought her small dog, Spike, to the vet, she was worried but unsure what was wrong. Spike, her usually vibrant 8-year-old Shih Tzu, had been acting a little sluggish, and something seemed off. He had lost the sparkle that once made him such a bundle of joy, and worst of all, his breath was unbearably smelly. She knew something wasn’t right, but she couldn’t quite put her finger on it.
The vet’s examination uncovered more than just a case of bad breath—Spike had advanced periodontal disease. His gums were inflamed, and several teeth were coated with tartar. The vet recommended bloodwork to rule out other issues, which fortunately came back normal. But dental x-rays painted a grim picture: several of Spike’s teeth were abscessed, and the damage was severe.
Faced with these findings, the vet recommended immediate treatment, including the removal of the abscessed teeth. Susan nervously agreed, knowing it was the best option for Spike. After the surgery, Spike began his recovery, aided by pain medication and antibiotics. The first few days were tough, but slowly, Susan noticed a change—Spike’s energy was returning.
Two weeks later, during a recheck, Susan had great news to report to her vet. Her once sluggish dog was back to his bouncy, bright-eyed self. The vet reassured her that with proper care, including a new routine of daily tooth brushing, dental chews, and regular cleanings, Spike’s periodontal disease could resolve.
Susan couldn’t believe how much of a difference it made. Spike’s sparkle had returned, and he was now pain-free. His story serves as a powerful reminder of how essential dental health is for our pets—and how easily it can be overlooked.
What is Periodontal Disease?
Periodontal disease is the condition of inflammation and infection that affects the tissues surrounding the teeth. These tissues include the gingiva, cementum, periodontal ligament, and alveolar bone, which together make up the periodontium. Periodontal disease begins with gingivitis, an inflammation of the gums, and if unchecked, can progress to periodontitis, where the inflammation spreads to the ligaments and bones supporting the teeth. If it becomes sufficiently advanced, the teeth loosen and may fall out or need extracting.

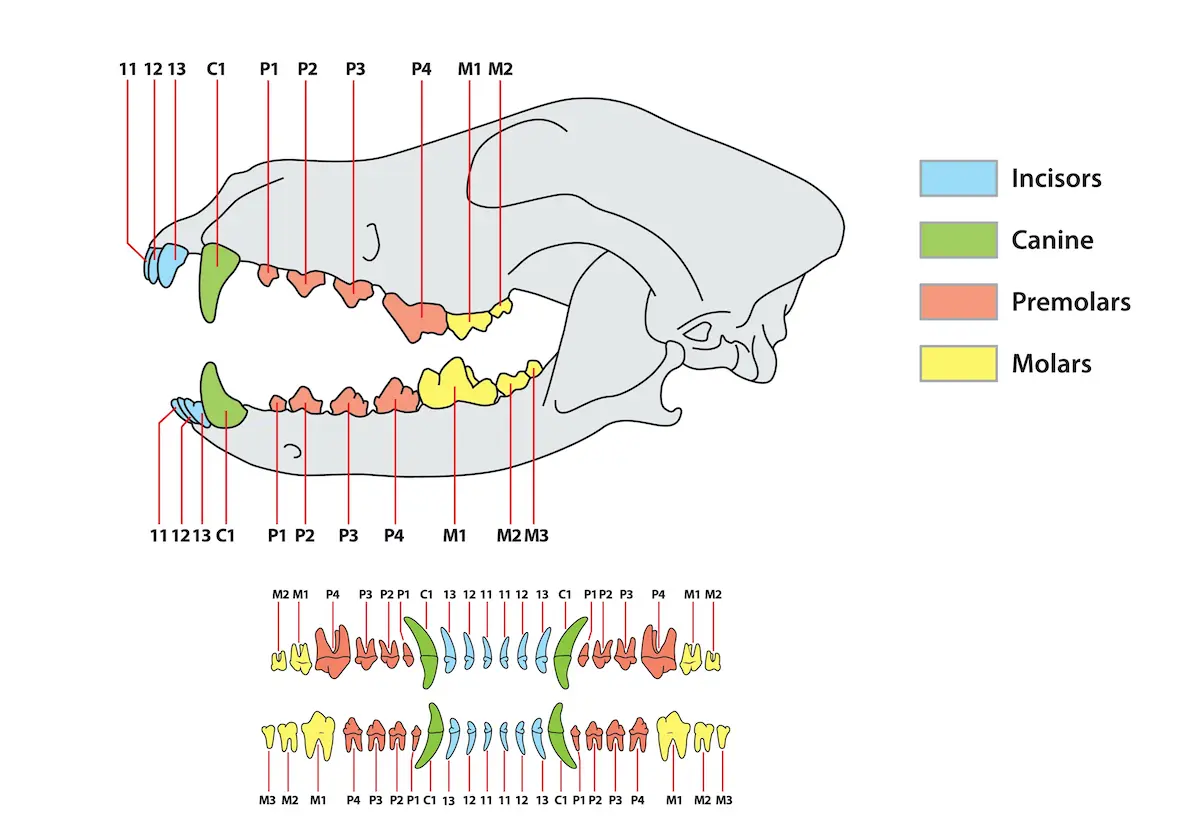
How Periodontal Disease Occurs
Plaque Formation:
- Bacteria and Food Particles: Plaque, a sticky biofilm composed of bacteria, food particles, and saliva, forms on the teeth after eating. The bacteria in plaque produce acids that can damage the enamel and irritate the gums. If not removed through regular scrubbing or brushing, plaque hardens into tartar within a few days.
Tartar Build-Up:
- Mineralization: Tartar, or dental calculus, is the mineralized form of plaque. It adheres strongly to the teeth and can only be removed by scaling (see “subgingival scaling”) or professional cleaning. Tartar provides a rough surface that facilitates further plaque accumulation and harbors bacteria, exacerbating gingivitis.
Gingivitis:
- Inflamed Gums: The first stage of periodontal disease is gingivitis, characterized by red, swollen gums. Mild gingivitis usually begins as a thin red line along the base of the teeth, becoming more noticeable and involving more of the gingiva as it worsens. Gingivitis occurs as a result of the body’s immune response to bacterial infection, and is often reversible with a combination of professional dental care and dedicated daily oral care.
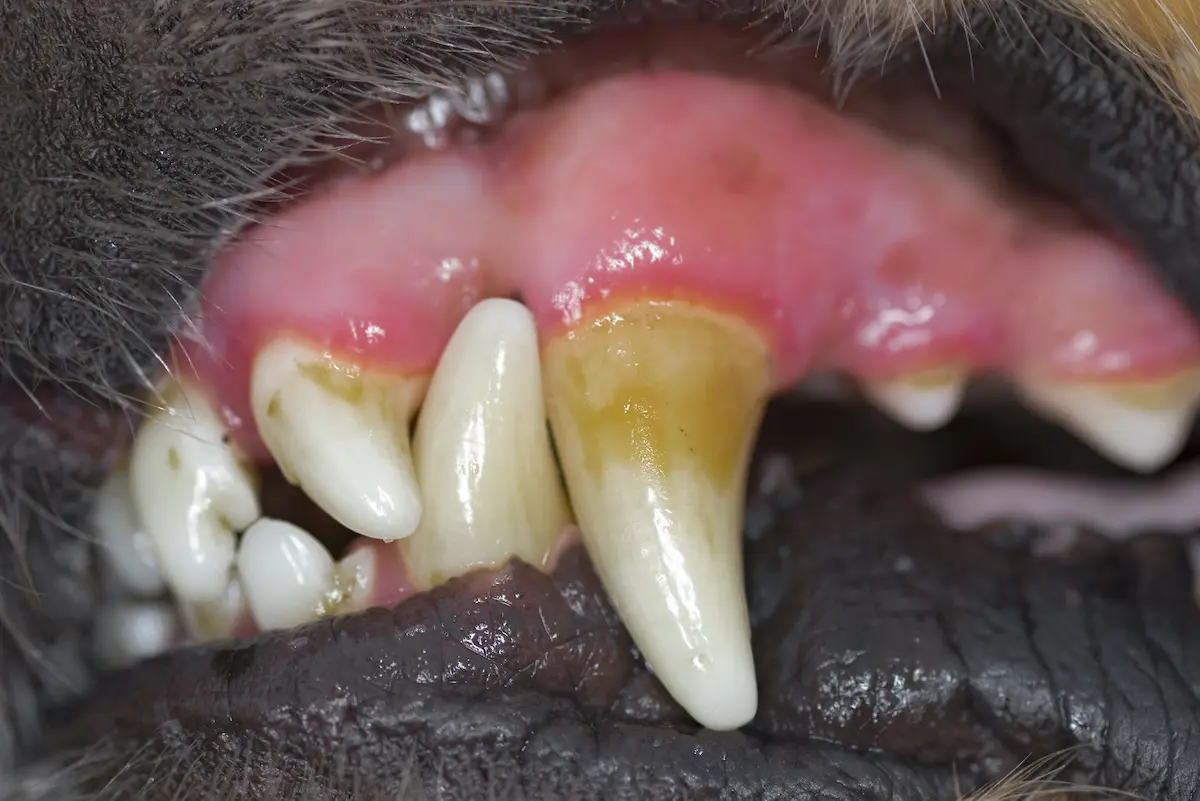
Periodontitis:
- Advanced Disease: If gingivitis is left untreated, it can progress to periodontitis, in which infection spreads to the periodontal ligament and alveolar bone supporting the teeth. This progression is due to the destruction of connective tissue and bone through the action of bacterial toxins and the host’s inflammatory response. The body’s attempt to fight the infection leads to further tissue destruction. At this stage, interventions such as dental extractions are necessary.
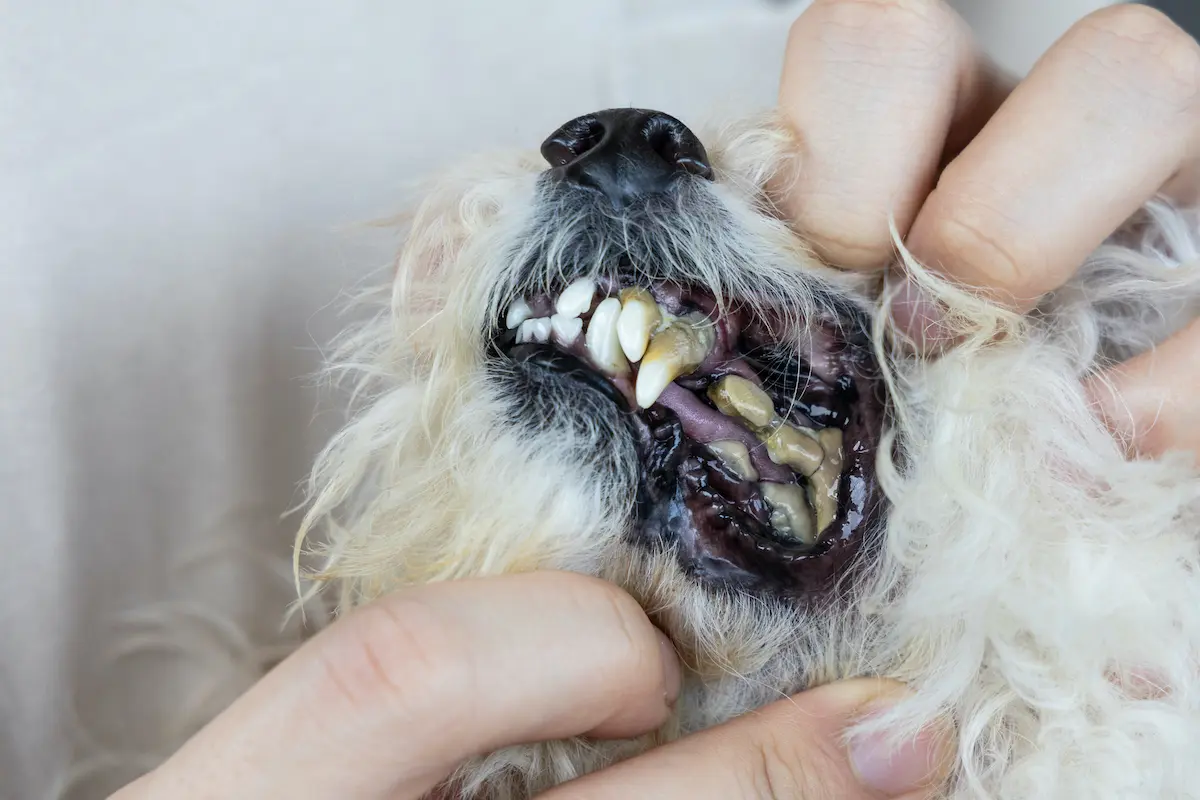
Causes and Risk Factors
Poor Oral Hygiene:
- Lack of Daily Oral Care: Regular brushing or scrubbing removes plaque and prevents tartar from mineralizing. If teeth are not cleaned, bacteria reproduce, plaque develops, and periodontal disease begins. Brushing mechanically disrupts the biofilm and reduces the bacterial load, helping to prevent gingivitis and periodontal disease.
- Lack of Professional Veterinary Cleaning Under Anesthesia: It is possible to do some dental cleaning in awake dogs, and this can be helpful at times for interim cleaning of the crowns (see “dental crowns”) of the teeth above the gumline.
- However, to prevent and treat periodontal disease, cleaning must be done under the gumline and completely into any periodontal pockets that may be present. Anesthesia is necessary to safely, comfortably and effectively perform thorough cleaning, or prophylactic dentistry (see “prophylactic dental cleaning”), according to the veterinary standard of care.
- If the teeth are not cleaned under anesthesia when necessary, and tartar is not removed from both above and below the gingival surface, periodontal disease is likely to start developing.
Diet:
- Soft Foods: Dogs fed primarily on soft foods are more prone to plaque accumulation compared to those on a diet that includes dry kibble, which can help mechanically clean the teeth through abrasion.
Age:
- Older Dogs: The immune system weakens gradually with age, thus allowing periodontal disease to develop more quickly in older dogs. Periodontal tissue is also slower to heal and regenerate in older dogs than in their younger counterparts.
Genetics:
- Breed Predisposition: Small breeds such as Miniature Dachshunds and Yorkshire Terriers are more prone to periodontal disease than large dogs because genetic factors can also influence the structure of the teeth and gums and the immune response to bacterial infection.
Other Health Conditions:
- Chronic Disease: Diseases such as diabetes can increase the risk of periodontal disease due to decreasing the body’s ability to fight infection. It is thought that the inhibited immune system in chronic disease allows the bacteria in the mouth to build up more than in a normal dog, causing periodontal disease earlier.
Other Dental Conditions:
- Malocclusions, Crowded Teeth, and Retained Deciduous Teeth: These can lead to periodontal disease through the tendency to develop increased plaque and tartar. The mechanisms of tongue movement, salivation, and food passage through the oral cavity are not functioning in a normal manner when the teeth are not situated in the normal place in the oral cavity. Abnormally placed teeth often chronically trap food, which leads to the rapid development of periodontal disease, if not addressed.
Medications:
- Immunosuppressive medications such as steroids can increase the tendency to develop periodontal disease, or allow a chronic situation to become acute, as it decreases the immune system’s ability to fight infections.

Symptoms of Periodontal Disease in Dogs
Halitosis:
- Persistent bad breath is often the first noticeable sign of periodontal disease. It is caused by volatile sulfur compounds (VSCs) produced by bacteria in the mouth.
Gingivitis:
- Inflammation of the gums that may be red and swollen due to increased blood flow and immune cell infiltration. Gingivitis is an early sign of periodontal disease.
Bleeding Gums:
- Gums that bleed easily, especially during brushing or eating, indicate gingivitis. Healthy gums do not bleed easily when brushed or rubbed.
Increased Salivation:
- Ptyalism, or increased salivation (drooling) can be a sign of oral discomfort or disease. Oral pain will often cause excess salivation.
Difficulty Eating:
- Dogs with periodontal disease may eat less, favor one side of their mouth, or drop food due to pain caused by inflamed or infected tissues, or abscessed or loose teeth.
Loose or Missing Teeth:
- Periodontal disease can cause teeth to become loose or fall out as the supporting structures are damaged or destroyed.
Pawing at the Mouth:
- Dogs in pain may paw at their mouth in an effort to soothe themselves or get relief.
Face Rubbing:
- Dogs with dental pain may rub their face to get relief.
Facial Swelling:
- If bacteria travel from the gingiva along gingival pockets to the tooth root, they can form an abscess. If present, a tooth root abscess often causes facial swelling. This is most commonly seen with an upper fourth premolar tooth root abscess, which typically causes swelling on the face below the eye.
- An abscess also commonly forms due to a fractured tooth.
- With a fractured tooth, bacteria enter through the pulp canal, and travel to the tooth root where an abscess develops.
Sneezing and/or Nasal Discharge:
- If the nasal cavity is involved because of a tooth root abscess or oronasal fistula, the dog may exhibit signs such as sneezing. If infection is present, there may be purulent nasal discharge.
Advertisement
Diagnosing Periodontal Disease
Awake Veterinary Examination:
- Your veterinarian will thoroughly examine your dog’s mouth as much as possible when they are awake. They will evaluate the amount and distribution of plaque and calculus, and check for halitosis and ptyalism. They will assess gingivitis and look for gingival bleeding, root exposure, parulides (a papule (see “papules”) on the gingiva indicative of a tooth abscess), loose or missing teeth, oral and nasal foreign bodies, nasal and ocular discharge, as well as any other abnormalities.
- They will also typically palpate the size and shape of local lymph nodes, as well as your dog’s heart, lungs, and general health, in preparation for an anesthetic veterinary examination or an anesthetic dental cleaning, if indicated.
- They may suggest a blood evaluation to check your pet’s general health and heartworm status.
Anesthetic Veterinary Examination:
- Full evaluation of your dog’s teeth and mouth can only be done when they are anesthetized. Once your dog is under anesthesia, your veterinarian will likely x-ray their teeth before cleaning or other procedures, then examine each tooth individually.
- A periodontal probe is used to measure the gingival attachment of each surface of the teeth, as in human dentistry.
- The degree of severity of periodontal disease relates to a single tooth, and is assigned based on several criteria.
- These criteria include the presence or degree of gingivitis, the presence or amount of loss of attachment of the teeth, and the visibility and degree of exposure of the furcation of tooth roots.
Dental X-Rays:
- X-rays help assess the extent of periodontal disease below the gum line, revealing bone loss and tooth root problems. Radiographic (see “radiography”) examination is crucial for a complete diagnosis as it shows changes that are not visible to the naked eye.
- X-rays assess tooth attachment loss, bone loss, loss of the lamina dura, widening of the periodontal ligament space, and resorption of the tooth root.
- They are also necessary for evaluating for tooth root abscesses.
Professional Cleaning:
- A thorough cleaning under anesthesia allows for the removal of tartar, assessment of the health of each tooth, and performing of necessary procedures such as extractions of abscessed or mobile teeth.
- Your veterinarian will likely recommend pre-anesthetic blood screening to help ensure your pet can safely tolerate anesthesia.
- Gas anesthesia with an endotracheal tube and proper monitoring ensures that the procedure can be performed safely, thoroughly, and pain-free. An endotracheal tube is a tube that is passed into the dog’s trachea, and connected to the gas anesthesia machine, delivering a specific mixture of oxygen and anesthetic gas. The veterinary standard of care requires that dogs be maintained on gas anesthesia with an endotracheal tube in place, which protects their airway, during dental cleaning and procedures.
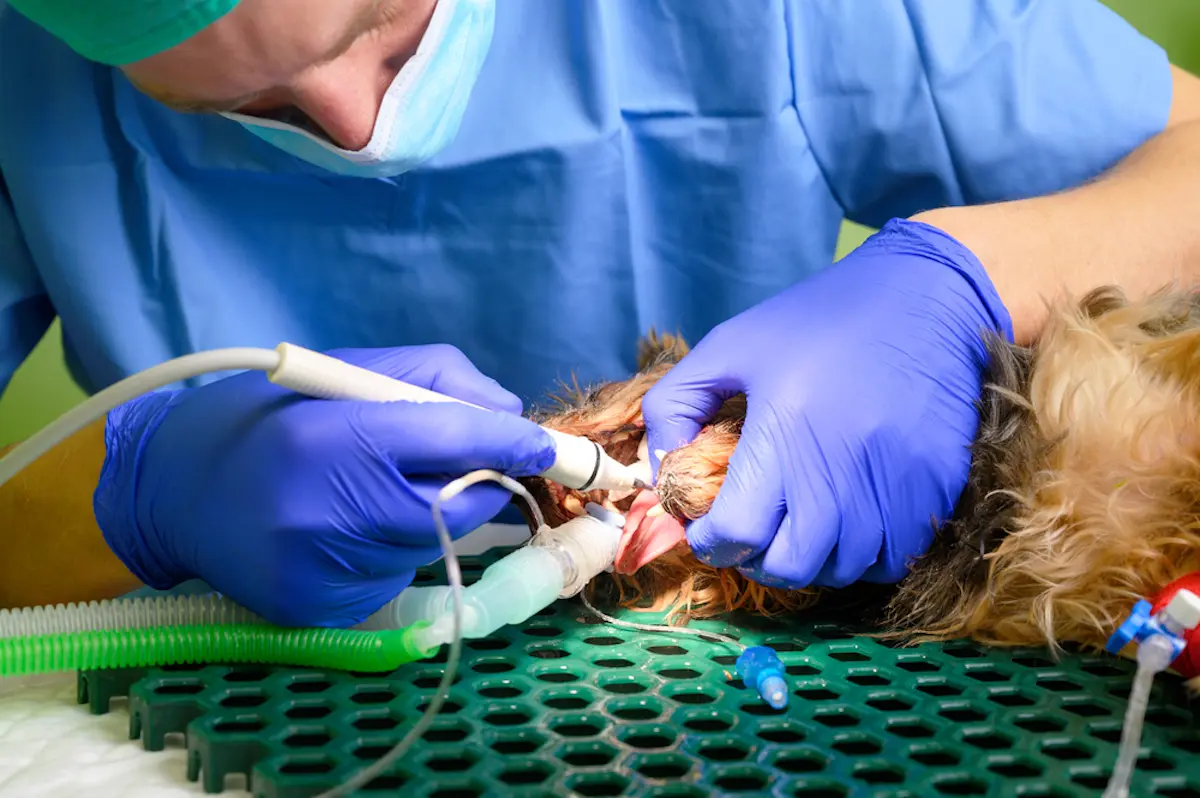
Preventing Periodontal Disease
Regular Brushing:
- Brushing your dog’s teeth daily is the most effective way to prevent plaque and tartar build-up. Brushing should ideally start in the first year of life. Use a dog-specific and properly sized toothbrush, and dog toothpaste, which is safe to be swallowed. The mechanical action of brushing disrupts the biofilm and removes food particles, helping to prevent plaque, tartar, and gingivitis. See our guide on how to brush your dog’s teeth here.
- If you are unable to brush your dog’s teeth, try dental finger brushes, finger socks, or gauze wrapped on your finger, to scrub your dog’s teeth and gums the best that you can.
- If that still doesn’t work for you, try an oral rinse or a water additive for your dog’s dental health.
Regular Veterinary Visits:
- Routine check-ups allow your veterinarian to catch dental issues early and provide timely treatment. Early intervention can prevent the progression of periodontal disease.
Professional Cleanings:
- Schedule regular dental cleanings with your veterinarian to remove tartar and check for signs of periodontal disease. For many dogs, yearly dental checkups and cleanings are adequate. Some larger dogs need them less frequently. For small dogs, especially as they get older, it is more common to need biannual checkups and cleanings.
Diet:
- Feeding your dog a diet designed for dental health can significantly reduce plaque and tartar formation. Chews: Chews can be helpful for the mechanical action of scrubbing plaque from the teeth before it hardens into tartar.
Chews:
- Chews can be helpful for the mechanical action of scrubbing plaque from the teeth before it hardens into tartar.
Toys:
- Toys can also be useful for some dogs in the prevention of periodontal disease through their mechanical action of scraping plaque and even tartar from the teeth. Rope toys and knobby toys are good examples of this.
Oral Rinses and Gels:
- Products like chlorhexidine rinses and dental gels can help control bacteria and inhibit plaque formation.

Treating Periodontal Disease
Professional Cleaning:
- Anesthetic dental cleaning (also called prophylaxis, or “prophy”), is the basis of periodontal treatment.
- X-rays are taken of the teeth while the dog is under anesthesia.
- The teeth are then scaled above and below the gingiva to remove all existing tartar, using a combination of ultrasonic and hand-scaling, depending on the situation.
- The teeth are then polished to ensure smooth surfaces.
- The veterinarian then examines the teeth and oral cavity thoroughly and addresses any concerns.
Antibiotics:
- Antibiotics may be prescribed to treat bacterial infections and reduce inflammation. They target specific bacteria and help manage infection, especially in severe cases. Antibiotics are generally given only if the underlying cause of the periodontal disease is addressed, not necessarily with every dental cleaning where gingivitis is present.
Extractions:
- In cases of advanced periodontal disease where there are abscessed teeth, mobile teeth, or tooth resorption, extraction of affected teeth is usually necessary to prevent further pain and treat infection.
Periodontal Surgery:
- Root planing, periodontal flaps, gingivectomy, gingivoplasty, and bone augmentation are all possible based on the severity and needs of the individual dog. Sometimes these procedures can be done on a referral basis at a dental specialty clinic after assessment at your regular veterinary clinic.
Home Care:
- After professional treatment, institute or continue a dental home care program to maintain your dog’s oral health. Consistent home care is essential to prevent recurrence and to achieve a successful outcome. If your dog has lost teeth due to periodontal disease, unless you institute a diligent home care program, it is very likely they will continue to lose their teeth.
Pain Management:
- Your dog may need pain control after their dental procedure. It is important to give pain medications on time without skipping doses, in order to avoid “getting behind the pain”, or having the pain be difficult to control.
Be sure to ask about post-dental pain control if your veterinarian does not mention it.
Advertisement
Conclusion
Periodontal disease in dogs is a common, multifactorial disease involving bacteria and the host’s immune response. It can be managed effectively with a combination of preventive care, including diligent daily toothbrushing, early detection with regular veterinary visits, and appropriate treatment with anesthetic dental cleanings, including appropriate periodontal procedures as needed. Diligent home dental care, regular veterinary visits, and professional cleaning, provide the cornerstone of good dental health for dogs. With this approach, periodontal disease can be managed effectively, ensuring that your canine companion remains healthy and happy.

 Pet News
Pet News